Data quality in healthcare means getting the medical details right. It is a simple definition, but achieving good data quality is complicated. Ensuring good healthcare data quality collection involves establishing clear rules through data governance, regular purging, and continuous monitoring based on guidelines.
But why is data quality in healthcare important? The answer lies in changing workflows in health systems. According to a HealthIT report, 78% of office-based physicians and 96% of non-federal acute care hospitals adopted a certified EHR as of 2021. The trend is only predicted to increase. As more EHRs replace paper records, there is a need to ensure data presented to patients and healthcare executives are accessible and complete. Hence, there is a need for good-quality data.
This brings us to data quality management (DQM), a critical aspect of maintaining the integrity and usefulness of healthcare data. This blog will discuss it and more related concepts to data quality in healthcare.
What is Data Quality Management in Healthcare?
The American Health Information Management Association defines data quality management as the business processes that ensure the integrity of an organization’s data during collection, application (including aggregation), warehousing, and analysis. It involves the processes, standards, and technologies to ensure data accuracy, access, completeness, relevance, timeliness, security, and consistency.
Failure to maintain quality can lead to multiple issues. The most common of them are:
- Inaccurate data in healthcare can result in misdiagnoses, compromising patient safety.
- Poor data quality hinders effective care coordination, leading to fragmented patient care.
- Healthcare professionals relying on unreliable data may make delayed or incorrect decisions, impacting treatment efficacy.
- Billing errors and coding discrepancies due to poor data quality pose financial implications for healthcare providers.
- Challenges in public health reporting arise, as poor data quality hampers accurate tracking of health trends.
- Patients may lose confidence in healthcare systems if they perceive data inaccuracies, leading to a breakdown in trust.
- Legal and compliance risks emerge with inaccurate or incomplete documentation, potentially resulting in litigation or regulatory penalties.
Different Formats of Healthcare Data
Healthcare data comes in various formats, each serving a unique purpose in patient care, administration, and research. Here is a summary table explaining them and where the information is utilized.
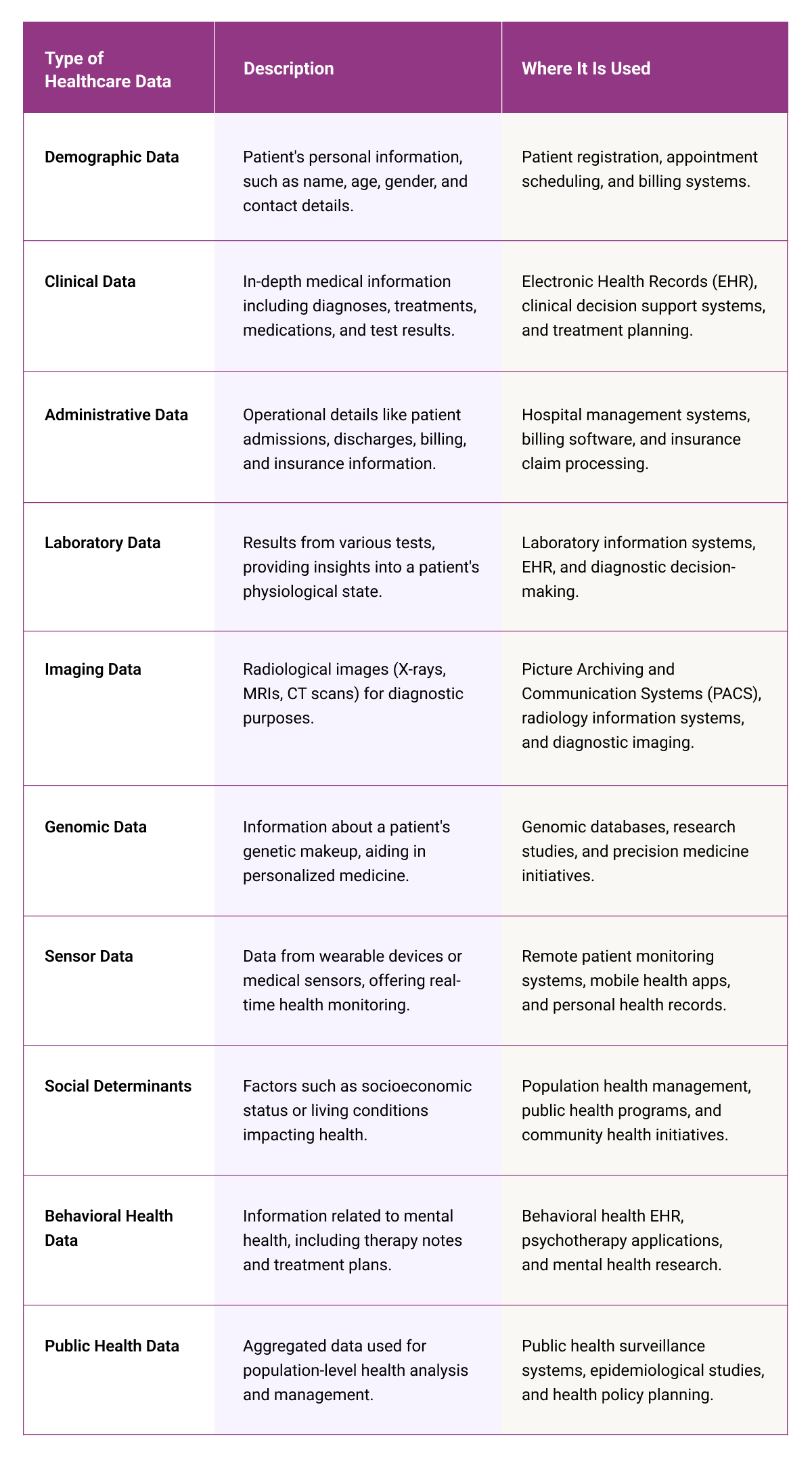
All of the data discussed above are susceptible to errors. From inaccurate entries and system malfunctions to questions on the reliability of the data. This is where the importance of good data collection comes into play. The secret lies in installing safeguards in the acquisition stage.
Safeguards to Improve Data Quality in Healthcare Systems
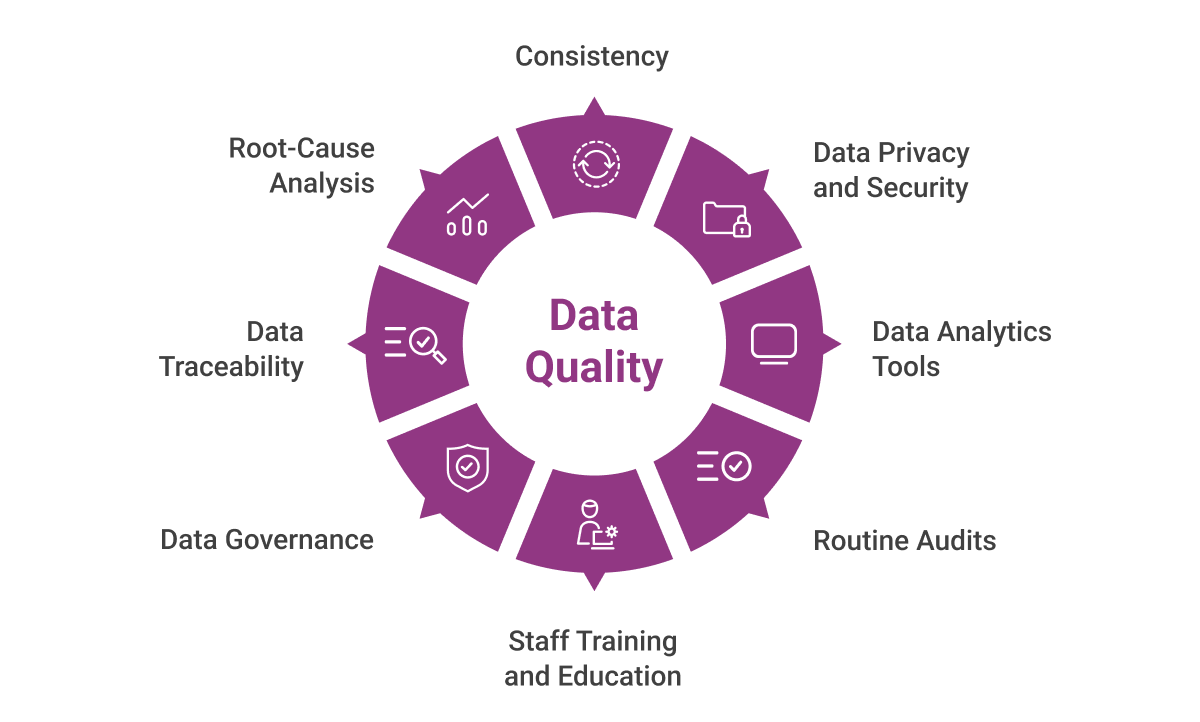
To enhance the quality of healthcare data, a strategic approach is essential. This section explores comprehensive methodologies aimed at fortifying data accuracy, security, and overall reliability.
1. Ensure Consistency Across Multiple Data Sources
This involves creating a smooth flow of information between everyone involved in a patient’s healthcare, from the lab to the doctor’s office or the hospital. Using standardized data formats, units, and terminology ensures the information’s accuracy. An example would be utilizing common coding systems, such as SNOMED CT for clinical terms and LOINC for laboratory results.
Similarly, adopting interoperability standards like Health Level Seven International (HL7) and implementing Fast Healthcare Interoperability Resources (FHIR) facilitates seamless data exchange between healthcare systems.
2. Protect Data Privacy and Security
Data protection needs to be a priority in the collection of patient information. This includes stringent access controls with role-based permissions, robust data protection encryption, and multi-factor authentication implementation to bolster login security.
The following are some security measures that are essential to protect privileged information:
- Implement stringent access controls and role-based permissions to restrict unauthorized entry.
- Utilize robust encryption methods to safeguard data both in transit and at rest.
- Enforce multi-factor authentication for heightened login security.
- Establish detailed audit trails to track and respond to access attempts systematically.
- Conduct regular security audits to identify and address potential vulnerabilities.
- Provide comprehensive user training to instill awareness and responsibility.
- Utilize data masking and anonymization techniques for added confidentiality.
- Ensure secure data transmission through protocols like HTTPS and VPNs.
- Establish clear contractual agreements with collaborators outlining data access restrictions.
- Develop and implement an incident response plan for swift and effective resolution of security breaches.
3. Implement Data Analytics Tools
With huge amounts of healthcare data being generated every day, managing the quality of the data for further usage is crucial. Integrating data analytics tools can significantly improve healthcare data quality management processes.
These tools help sort, store, and organize quality data, detect patterns, correct anomalies, and facilitate continuous monitoring and feedback loops. Caregivers, hospitals, and decision-makers can access and utilize the data generated.
4. Conduct Routine Audits
Every data requires regular health checks to ensure that the information is reliable enough for use. Regular audits help identify data discrepancies and maintain high data quality. This can be ensured by:
- Establishing a consistent audit schedule.
- Considering and evaluating the criticality of the data.
- Defining key data quality metrics, including accuracy, completeness, and timeliness.
These metrics serve as benchmarks, and when thresholds are exceeded, corrective actions are triggered to uphold data quality standards.
5. Undertake Staff Training and Education
For healthcare professionals, ongoing training programs ensure awareness regarding the importance of following data entry best practices. Ongoing staff education, integrated into new employee onboarding processes, is crucial for making the staff well-versed in accurate data documentation. Awareness campaigns can further reinforce the significance of data quality in positively impacting patient care.
6. Data Governance is Crucial
Effective data governance in healthcare involves the development of comprehensive policies covering data quality, privacy, and security. A clear definition of data ownership and accountability within the organization is vital. This can be achieved by appointing data stewards responsible for overseeing specific data domains and establishing a data governance council to review and approve data-related policies.
7. Ensure Data Traceability
Data traceability can be obtained by implementing unique identifiers for patients, healthcare providers, and other entities. Master Data Management (MDM) strategies can assign and maintain consistent identifiers across systems. Change tracking mechanisms, including robust audit trails, record all modifications to healthcare data, ensuring transparency and accountability.
8. Perform Root-Cause Analysis for Health Data Errors
Conducting root-cause analysis when data errors are identified is essential for understanding and addressing underlying issues. This structured process involves cross-functional teams, including IT, clinical staff, and data stewards, to investigate the causes of errors.
Based on the findings of the analysis, corrective action plans are developed and implemented, encompassing process improvements, additional training, or system enhancements to prevent similar errors in the future. Continuous monitoring is essential to ensure the effectiveness of these corrective actions.
Benefits of Focussing on Data Quality

Giving a laser-eyed focus on data quality is crucial for success in healthcare institutions. We have listed the most prominent among the many advantages below:
1. Informed Decision-Making
Accurate and reliable data is essential for healthcare professionals to make informed decisions about patient care. Mistakes or inaccuracies in the data can lead to incorrect diagnoses and treatment plans.
2. Efficient Healthcare Delivery
Quality data enhances the efficiency of healthcare delivery by ensuring that relevant information is available when and where it is needed. This is particularly important in emergencies and for coordinating care among different providers.
3. Ensuring Patient Safety
Incorrect or incomplete data can jeopardize patient safety. For example, medication errors may occur if healthcare providers do not have access to up-to-date and accurate information about a patient’s medical history and current medications.
4. Aiding Medical Research
Researchers rely on high-quality healthcare data for studies and clinical trials. Improving data quality enhances the validity and reliability of research findings, contributing to advancements in medical knowledge and treatment options.
5. Essential for Compliance and Reporting
Adherence to regulatory requirements and standards is crucial in healthcare. Accurate data is necessary for compliance with regulations and facilitates transparent reporting for auditing and quality improvement purposes.
How Rockit Helps Overcome Data Quality Issues in Healthcare
By combining deep expertise in FHIR and HL7 with a robust development approach, Rockit empowers healthcare organizations to navigate the complexities of data integration, ensuring the delivery of reliable and standardized health information for informed decision-making.
A Rockit partnership is a great step to ensure good data quality. We come with years of expertise in FHIR (Fast Healthcare Interoperability Resources) and HL7 (Health Level Seven) standards.
Leveraging a stringent development process, Rockit brings knowledge, ensuring that healthcare data is accurate and seamlessly interoperable across systems. We also have a proven track record of successful client deliveries.
To join our waitlist for a consultation, visit www.rockitteam.com/contact-us

